Diabetic Retinopathy Treatment in Ahmedabad
What is Diabetic Retinopathy?
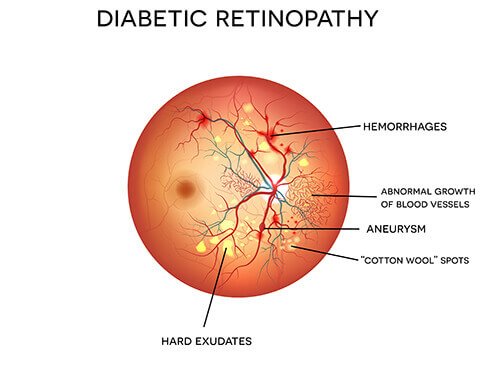
Diabetic retinopathy is a complication of diabetes that damages the retina, the light-sensitive layer at the back of the eye that converts what you see into signals sent to the brain. High blood sugar levels sustained over time gradually destroy the tiny blood vessels that supply the retina. These vessels may leak fluid, swell, or grow abnormally, progressively impairing vision in ways that are often not noticed until the damage is already significant.
Anyone with Type 1 or Type 2 diabetes can develop diabetic retinopathy. The longer a person has lived with diabetes and the less controlled their blood sugar has been, the greater the risk. Because the condition frequently develops without noticeable symptoms until it reaches an advanced stage, annual dilated eye examinations are essential for every person living with diabetes, regardless of how well their vision feels.
Diabetic retinopathy can also lead to a related condition called Diabetic Macular Oedema, in which fluid leaks from damaged vessels and accumulates at the macula, the central area of the retina responsible for sharp detail. Both conditions are manageable when identified in time. For a broader overview of retinal care at our centre, see our page on retinal treatment in Ahmedabad.
Diabetic retinopathy is particularly difficult to detect on your own because it causes no pain and minimal visual disturbance in its early stages. By the time symptoms become obvious, significant retinal damage may already have occurred. Understanding what to look for, what drives the condition, and what can go wrong without treatment helps explain why regular monitoring is not optional for people with diabetes.
Use the tabs below to explore the symptoms, causes, and potential complications of diabetic retinopathy.
Symptoms of Diabetic Retinopathy
In the early stages, diabetic retinopathy usually causes no symptoms at all. As it progresses, you may notice the following:
- Floaters: small dark spots, threads, or cobweb-like shapes that drift across the visual field
- Blurred vision that may come and go or worsen gradually over time
- Dark or empty areas in part of the visual field
- Difficulty seeing clearly at night or in low light conditions
- Colours that appear washed out or less vivid than usual
- Sudden, significant loss of vision, which is a medical emergency and requires urgent assessment
Causes and Risk Factors for Diabetic Retinopathy
Diabetic retinopathy develops when persistently high blood sugar damages the blood vessels supplying the retina. Several factors increase the risk or accelerate progression:
- Type 1 or Type 2 diabetes, both of which carry significant risk when the condition is longstanding or poorly controlled
- Poor blood sugar control, where persistently elevated HbA1c accelerates retinal vessel damage over time
- High blood pressure, which puts additional strain on already-vulnerable retinal vessels
- High cholesterol, which contributes to lipid deposits in the retina and worsens the extent of vessel damage
- Diabetic kidney disease (nephropathy), which is associated with more severe retinopathy
- Pre-existing diabetes during pregnancy, as hormonal changes can accelerate retinopathy progression
- Smoking, which worsens blood vessel health and accelerates diabetic complications throughout the body
Complications of Untreated Diabetic Retinopathy
Without timely treatment, diabetic retinopathy can progress to sight-threatening complications:
- Vitreous haemorrhage: abnormal new blood vessels leak into the vitreous gel inside the eye, causing sudden blurring or a dramatic drop in vision
- Tractional retinal detachment: scar tissue from abnormal vessel growth contracts and pulls the retina away from the back of the eye, threatening permanent vision loss
- Neovascular glaucoma: new blood vessels growing on the iris and drainage structures of the eye raise eye pressure and damage the optic nerve
- Diabetic Macular Oedema: fluid accumulating at the macula directly impairs reading vision and the ability to see fine detail
- Permanent vision loss in advanced or neglected cases where retinal and macular damage has become irreversible
Stages of Diabetic Retinopathy
Diabetic retinopathy is classified into four main stages. The stage at diagnosis determines which treatment approach is most appropriate and how urgently it needs to begin.
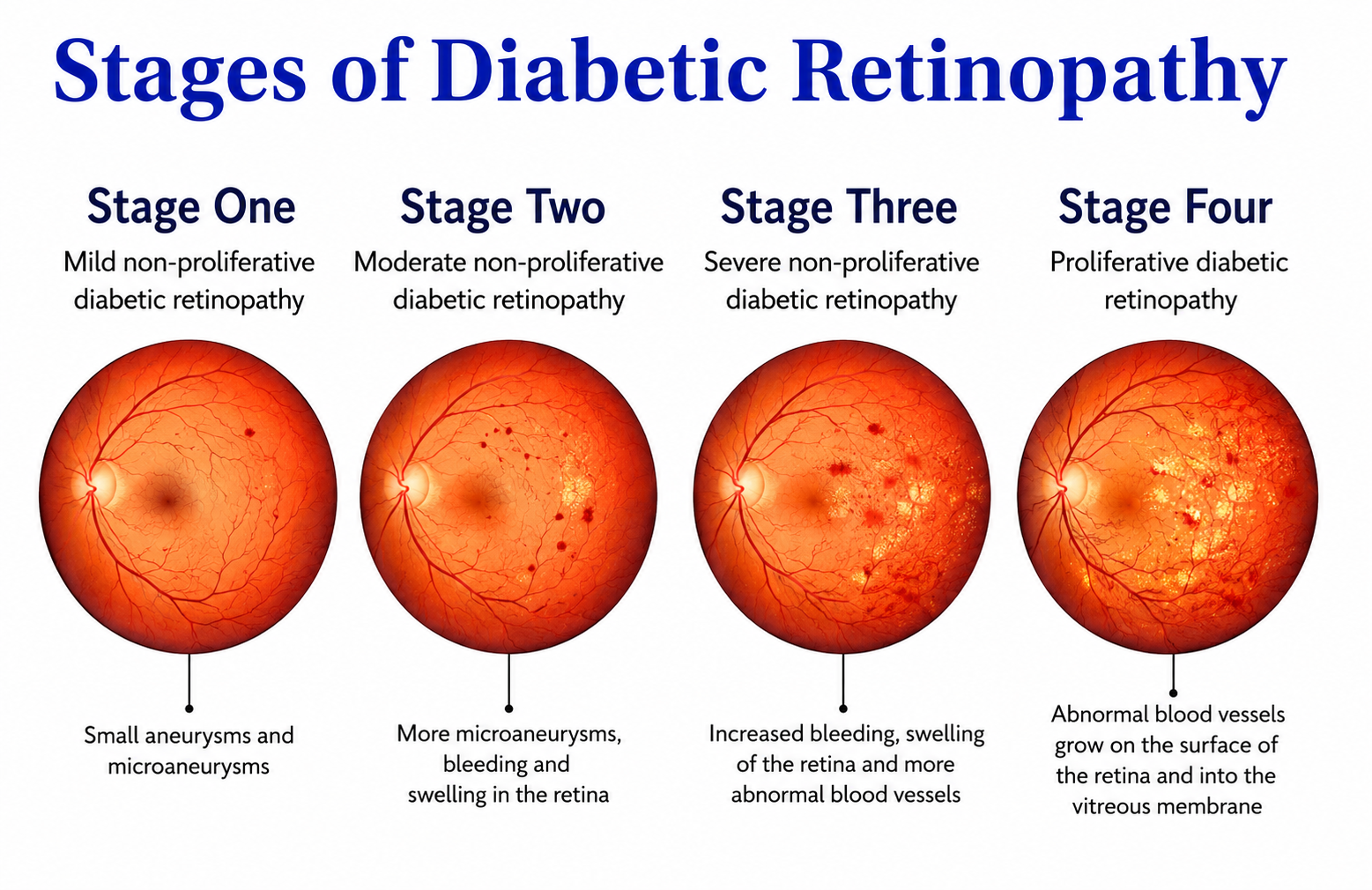
Stage 1: Mild Non-Proliferative DR
Tiny balloon-like swellings called microaneurysms appear in the retinal blood vessels. This is the earliest detectable stage and most people have no symptoms. Close monitoring with OCT and fundus photography is recommended. No active treatment is usually required at this stage, but the frequency of review depends on overall diabetes control.
Stage 2: Moderate Non-Proliferative DR
More blood vessels become blocked, reducing blood flow to areas of the retina. Changes become more visible on imaging. Some patients begin to notice mild blurring, particularly if the macula is affected. Review every three to six months is important to catch any deterioration early.
Stage 3: Severe Non-Proliferative DR
Large areas of the retina are deprived of adequate blood supply. The retina begins producing signals that stimulate abnormal vessel growth. No new vessels have formed yet, but the risk of progression is high without close monitoring and, in many cases, treatment.
Stage 4: Proliferative DR
Abnormal new blood vessels grow on the surface of the retina or into the vitreous gel. These fragile vessels bleed easily, causing floaters or sudden vision loss. Scar tissue can form and pull on the retina. This is the highest-risk stage and requires prompt treatment to prevent permanent damage.
Diabetic Macular Oedema: A Separate but Related Condition
Diabetic Macular Oedema can develop at any stage of retinopathy, not only in advanced cases. It occurs when fluid leaks from damaged blood vessels and builds up at the macula, the small central area of the retina responsible for sharp, detailed vision. It is the most common cause of vision impairment in people with diabetic retinopathy and is typically treated with anti-VEGF injections, separately from the underlying retinopathy.
Treatment Options for Diabetic Retinopathy in Ahmedabad
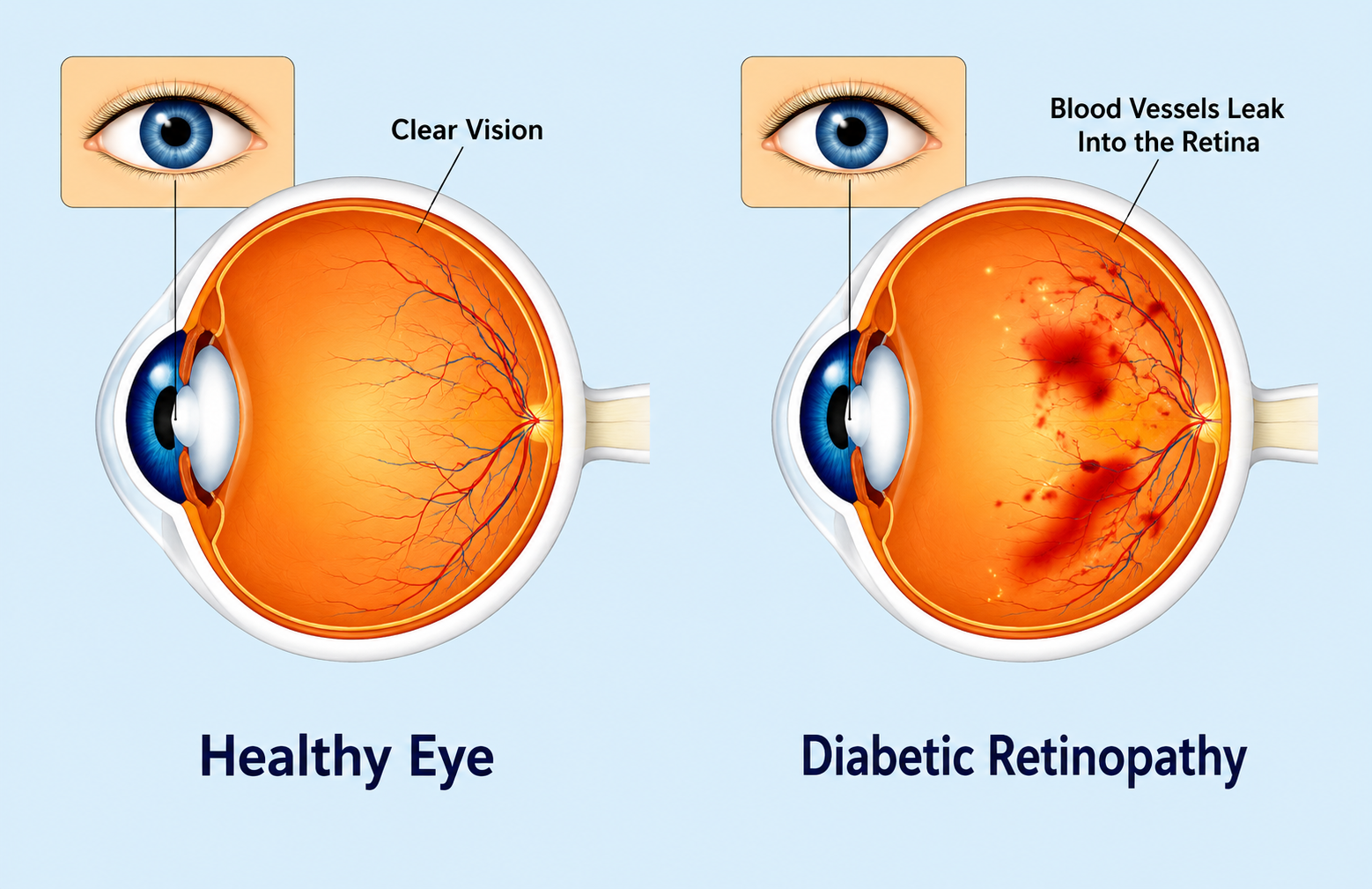
The right treatment depends on the stage of retinopathy and whether Diabetic Macular Oedema is also present. At Krisha Eye Hospital, every patient undergoes a thorough retinal assessment before any treatment is recommended. Complex cases often require a combination of approaches used in sequence as the condition evolves.
Anti-VEGF Injections
The first-line treatment for Diabetic Macular Oedema and Proliferative DR. Medicines including bevacizumab, ranibizumab, and aflibercept are injected directly into the eye to block the chemical signal that drives abnormal vessel growth and fluid leakage. A course of monthly injections is typically given initially, with the interval extended over time depending on the response.
Laser Photocoagulation
Focal or grid laser treatment targets leaking blood vessels to reduce fluid at the macula in DME. Panretinal Photocoagulation (PRP) uses a broader pattern of laser spots to treat severe non-proliferative and proliferative DR by reducing the stimulus for new vessel growth. Both procedures are performed in the clinic without general anaesthesia.
Vitrectomy
A surgical procedure performed in the operating theatre for advanced proliferative DR. The vitreous gel is removed along with any blood that has leaked into it, and scar tissue causing tractional retinal detachment is carefully released. Vitrectomy can restore useful vision in cases where other treatments are no longer sufficient to manage the condition.
Steroid Injections and Implants
For Diabetic Macular Oedema that does not respond adequately to anti-VEGF therapy, intravitreal steroid injections or sustained-release implants such as dexamethasone implants may be used. They reduce inflammation and fluid accumulation at the macula. Patients on steroid therapy are monitored for raised eye pressure, which can occur as a side effect.
Diabetic Eye Monitoring
For mild non-proliferative DR without Macular Oedema, active treatment may not be required immediately. A structured monitoring programme using OCT and fundus photography tracks any changes every three to six months, so treatment can begin as soon as it is genuinely needed, before vision is affected.
Combined Treatment Approach
Cases where both Diabetic Macular Oedema and Proliferative DR are present often respond best to a combination of treatments used in the right order. This may involve a course of anti-VEGF injections first to stabilise new vessel growth, followed by laser photocoagulation, with vitrectomy reserved for cases that do not respond adequately. Your plan at Krisha Eye Hospital is matched to your specific retinal findings.
Before, During and After Treatment
Before Your Treatment
Inform your doctor of all diabetes medications you are currently taking, including insulin and oral tablets, as these may need to be considered around the time of certain procedures. Blood sugar control in the days before treatment matters: better-controlled blood sugar at the time of any retinal intervention is associated with improved outcomes. You will need a dilated eye examination before treatment, and your vision will be temporarily blurred afterwards, so arrange for someone to accompany you home. OCT imaging and fundus photography are used to map the retina and measure any fluid or swelling. If fluorescein angiography is needed, a small amount of dye is injected into a vein in the arm to highlight any blood vessel leakage. Let your doctor know of any known allergies before this test is performed.
During Your Treatment
Anti-VEGF injections and laser photocoagulation are both performed in the clinic with no hospital admission required. Before an injection, the eye is numbed with anaesthetic drops and a small speculum keeps the eyelid open comfortably. The injection itself takes under five minutes. During laser treatment, you may notice flashes of light and a mild stinging sensation, and the session typically lasts 15 to 30 minutes depending on the area being treated. Vitrectomy is performed in the operating theatre under local or general anaesthesia depending on your individual circumstances, and patients return home on the same day in most cases.
After Your Treatment
Antibiotic and anti-inflammatory eye drops will be prescribed after injection or surgery, and it is important to complete the full course as directed. Anti-VEGF injections are given monthly initially, with the interval extended based on how the macula responds over time. A typical follow-up schedule involves a review at one month, then three months, and then every three to six months depending on your stage and treatment response. Maintaining good blood sugar control after treatment significantly improves long-term outcomes. Report any sudden increase in floaters, new flashes of light, or a significant drop in vision immediately, as these may indicate a complication that needs urgent review.
Why Choose Krisha Eye Hospital for Diabetic Retinopathy Treatment in Ahmedabad?
- Advanced diagnostic equipment including OCT, digital fundus photography, and fluorescein angiography available on-site for accurate retinal assessment
- Timely anti-VEGF injections with minimal waiting, as delays in treatment for active DME or proliferative DR can result in avoidable vision loss
- In-clinic laser photocoagulation including focal, grid, and panretinal patterns, with no need for referral elsewhere for standard procedures
- Surgical options including vitrectomy for advanced cases, discussed transparently and only recommended when genuinely indicated
- Coordinated care approach: we communicate with your diabetologist and general physician to ensure your diabetes management and eye care are aligned
- Clear, honest cost estimates provided during your consultation with no hidden charges at any stage of your care
- Convenient location near Vaishnodevi Circle, Ahmedabad, with easy access for patients across the city and surrounding areas
Prevention Tips for Diabetic Eye Disease
Diabetic retinopathy cannot always be prevented entirely, but these steps significantly reduce the risk of progression and vision-threatening complications.
- Have a dilated eye examination at least once a year, even when your vision seems completely normal. Early diabetic retinopathy causes no symptoms, and only a clinical examination can detect it reliably.
- Keep your HbA1c within the target range recommended by your diabetologist. Good blood sugar control is the single most effective way to protect your retinal vessels over the long term.
- Control blood pressure. High blood pressure speeds up retinal vessel damage in people with diabetes and makes existing retinopathy progress faster.
- Manage cholesterol levels. Lipid deposits in the retina are associated with more difficult-to-treat changes at the macula and are more common when cholesterol is poorly controlled.
- Stop smoking. Smoking worsens blood vessel health throughout the body and accelerates every diabetic complication, including retinopathy.
- Follow a healthy diet and maintain regular physical activity to support overall diabetes management and reduce systemic risk factors.
- Report any change in vision promptly. Floaters, blurring, or dark patches in your visual field should be assessed by an eye specialist, not monitored at home.
- Work closely with both your diabetologist and eye specialist. Coordinating care between both teams gives you the best chance of protecting your vision over the long term.
What Our Patients Say
These are real experiences shared by patients who came to Krisha Eye Hospital for diabetic retinopathy treatment in Ahmedabad.
"I have had Type 2 diabetes for over twelve years and my vision always felt fine, so I never thought to get my eyes checked separately from my routine blood tests. My physician finally suggested a diabetic eye check-up at Krisha Eye Hospital and I am glad I went. They found moderate non-proliferative retinopathy in my right eye with early fluid at the macula. The doctor was very thorough in explaining what it meant and what would happen if I left it. I started on anti-VEGF injections and my last OCT scan showed a significant reduction in fluid. My vision is stable and I have no discomfort. I had no idea this was developing behind the scenes and I would have done nothing if it were not for that referral."
"I noticed blurring when reading about six months before I came to Krisha Eye Hospital. I had assumed it was just my age or my existing glasses prescription needing a change. The doctor here did a proper OCT scan on the first visit and found significant fluid at the macula from diabetic macular oedema. She explained clearly that changing my glasses would not fix this and that the blurring was coming from the fluid, not the lens. I had three anti-VEGF injections over the following months and the fluid reduced considerably each time. I can now read comfortably again. The whole team was very patient and the doctor always took the time to explain my scan results before and after each injection."
"I woke up one morning with a large dark floater and my vision on one side had dropped almost overnight. I came to Krisha Eye Hospital the same day. They found a vitreous haemorrhage from proliferative diabetic retinopathy. I will be honest, I had known my blood sugar was not well controlled but had not been getting my eyes checked regularly. The doctor explained what had happened without making me feel judged and outlined exactly what treatment was needed. I had laser photocoagulation and anti-VEGF injections. The blood gradually cleared over the next few weeks and most of my vision returned. I am now on a strict monitoring schedule and, more importantly, I have taken my blood sugar management much more seriously. The experience was a warning I needed to hear."
"My husband has had diabetes for many years and I bring him to Krisha Eye Hospital every year for his diabetic eye check-up. Last year they found Grade 3 retinopathy and recommended laser treatment promptly. The procedure itself was quick and he was home the same day. His follow-up scans have shown good stability since the laser was done. What I appreciate most about the team here is that they are honest about what is found and what needs to be done. They explain everything clearly to both of us, not just to the patient. We feel confident that he is being monitored properly and that any change will be caught in time."
Our Doctor
Questions about diabetic eye disease are best answered in person with a full retinal assessment. Dr. Dhwani Maheshwari and the team at Krisha Eye Hospital evaluate every diabetic patient carefully to ensure nothing is missed at any stage of their care.

Dr. Dhwani Maheshwari
Cataract & Refractive Surgeon | Krisha Eye Hospital, Ahmedabad
Dr. Dhwani Maheshwari completed her DOMS from Civil Hospital Ahmedabad and has performed more than 5,000 eye surgeries. She leads comprehensive eye care at Krisha Eye Hospital, including diabetic retinopathy screening and management across all stages. Her approach begins with a thorough retinal evaluation, followed by a treatment plan that is honest about what is needed and why.
Book ConsultationFrequently Asked Questions
Can diabetic retinopathy be cured?
Diabetic retinopathy cannot be reversed. Once retinal cells are damaged, they do not regenerate. However, treatment can halt progression and preserve the vision you still have. In cases of Diabetic Macular Oedema, anti-VEGF therapy can sometimes achieve a meaningful improvement in vision if started before irreversible damage has occurred. Early detection remains the single most important factor in protecting sight, which is why annual diabetic eye examinations are essential even when vision feels completely normal.
How often should a person with diabetes get an eye check-up?
At a minimum, once a year, even if vision seems perfectly normal. Because diabetic retinopathy can be present and progressing without any noticeable symptoms, a dilated eye examination is the only reliable way to detect it early. If retinopathy has already been diagnosed, your doctor may recommend review every three to six months depending on the stage and whether Diabetic Macular Oedema is present.
Is anti-VEGF injection treatment painful?
The eye is numbed thoroughly with anaesthetic drops before the injection is given. Most patients feel only mild pressure during the procedure, which takes under five minutes. A gritty or mildly uncomfortable sensation may persist for a few hours after the injection but settles on its own. Significant pain after an injection is uncommon and should be reported to your doctor promptly if it occurs.
Can vision lost to diabetic retinopathy be restored?
Vision loss from advanced retinopathy or longstanding macular oedema may not be fully reversible once significant damage has occurred. However, in cases where treatment begins before major damage has taken place, vision can often be stabilised and, in some DME cases, partially improved with anti-VEGF therapy. This is why the emphasis at every stage is on early intervention rather than waiting for symptoms to appear.
What is the cost of diabetic retinopathy treatment in Ahmedabad?
Costs vary depending on the treatment required. Diagnostic examinations including OCT and fundus photography are priced separately from treatment procedures. Anti-VEGF injections, laser photocoagulation, and vitrectomy each carry different costs, and the number of sessions or injections needed varies between patients. Krisha Eye Hospital provides a clear, itemised cost estimate during your first consultation with no hidden charges at any stage. Contact us to arrange an assessment.
Does controlling blood sugar stop diabetic retinopathy from getting worse?
Good blood sugar control significantly slows the progression of diabetic retinopathy and substantially reduces the risk of vision-threatening complications. Large clinical studies including the Diabetes Control and Complications Trial and the UK Prospective Diabetes Study have confirmed that tight glycaemic control reduces the development and worsening of retinopathy. However, once retinopathy has reached moderate or severe stages, medical or laser treatment is typically still required alongside blood sugar management, as blood sugar control alone is usually not sufficient at these stages.
Is diabetic retinopathy treatment a one-time procedure?
No. Managing diabetic eye disease is an ongoing process rather than a single intervention. Anti-VEGF injections are typically given as a series of monthly injections initially, with the interval extended based on your response over time. Laser treatment may require more than one session. Regular monitoring continues long-term regardless of which treatment is used. Because the underlying cause is diabetes, the retina remains at risk and must be reviewed consistently throughout life.
Protecting Your Vision Starts with One Appointment
Book a diabetic eye check-up at Krisha Eye Hospital, Ahmedabad. Early detection makes all the difference.
2nd Floor, Shaligram Lakeview Commercial, near Vaishnodevi Circle, Ahmedabad 382421 | +91 75677 67701
Related Treatments at Krisha Eye Hospital
Explore other services offered by our team in Ahmedabad.
Contact Us For Any Further Question
Address 2nd Floor, Shaligram Lakeview Commercial, near Vaishnodevi Circle, Ahmedabad 382421
Phone +91 75677 67701
Hours Mon–Sat: 10:30 AM – 1:30 PM & 6:00 PM – 7:30 PM
Medical Disclaimer: The information on this page is provided for general educational purposes only and does not constitute medical advice. Diabetic retinopathy is a clinical condition that requires assessment and diagnosis by a qualified ophthalmologist. Treatment recommendations vary based on individual clinical findings. Please consult a doctor before making any decisions about your eye health or diabetes management. Krisha Eye Hospital, Ahmedabad.
