Diabetic Retinopathy: Early signs you should never ignore
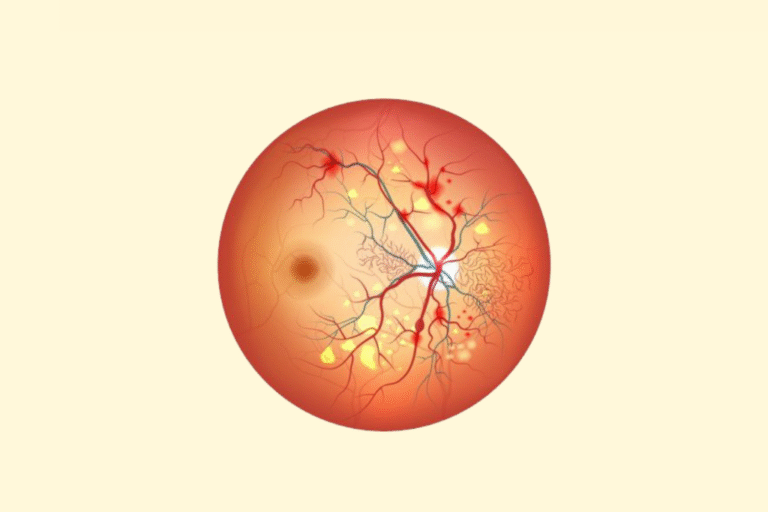
Diabetes affects millions of people worldwide and, while most understand its impact on the heart, kidneys, and nerves, fewer are aware of its silent threat to vision. One of the most common eye complications caused by diabetes is diabetic retinopathy—a condition that can gradually lead to blindness if not detected and treated in time.
The frightening part? Diabetic retinopathy often develops without noticeable symptoms in the early stages. By the time vision loss occurs, significant and sometimes irreversible damage has already happened. That’s why knowing the early warning signs is crucial.
This blog will help you understand what diabetic retinopathy is, its risk factors, the early signs you should never ignore, and the steps you can take to protect your eyesight.
Table of Contents
ToggleWhat is diabetic retinopathy?
Diabetic retinopathy is a complication of diabetes that damages the tiny blood vessels in the retina—the part of your eye responsible for capturing images and sending them to your brain.
When blood sugar levels remain high for long periods, these delicate vessels may:
- Leak fluid or blood into the retina,
- Swell and distort vision, or
- Close off completely, cutting off blood supply.
In advanced stages, abnormal new blood vessels may form, which are fragile and prone to bleeding. Over time, scar tissue can build up, increasing the risk of retinal detachment and blindness.
Types of diabetic retinopathy
There are two main stages:
- Non-Proliferative Diabetic Retinopathy (NPDR):
- Early stage where small retinal blood vessels leak fluid or tiny amounts of blood.
- May cause swelling of the retina (macular edema), leading to blurred vision.
- Often has no symptoms at first, which makes regular eye exams essential.
- Early stage where small retinal blood vessels leak fluid or tiny amounts of blood.
- Proliferative Diabetic Retinopathy (PDR):
- Advanced stage where abnormal blood vessels grow on the retina.
- These vessels are fragile and can bleed, causing severe vision loss.
- May lead to retinal detachment or glaucoma.
- Advanced stage where abnormal blood vessels grow on the retina.
Early signs you should never ignore
Recognizing the early signs of diabetic retinopathy can make the difference between saving and losing your vision. Even mild changes in vision should be taken seriously.
1. Blurred or Distorted Vision

- One of the first signs of retinal swelling caused by fluid leakage.
- May come and go, often mistaken for needing new glasses.
2. Floaters in vision

- Small spots, strings, or cobweb-like shapes drifting in your line of sight.
- Caused by bleeding into the vitreous (gel-like fluid inside the eye).
3. Difficulty seeing at night

- Trouble adjusting your eyes to low-light conditions.
- Can make activities like driving in the evening increasingly difficult.
4. Fluctuating vision

- Vision may appear sharp one day and blurred the next.
- High blood sugar levels affect the eye’s fluid balance, temporarily changing focus.
5. Dark or Empty spots in vision

- ndicates areas of the retina are not receiving enough blood supply.
- May start as small blind spots and worsen over time.
6. Faded or Altered color vision
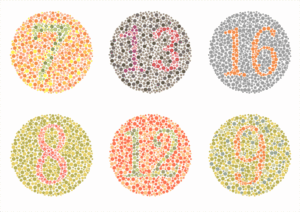
- Colors may seem duller or harder to distinguish.
- Suggests retinal damage is interfering with how the eye processes light.
Why is early detection crucial?
The most dangerous aspect of diabetic retinopathy is its silent progression. In the early stages, there may be no pain and very few noticeable symptoms. By the time vision problems appear, significant retinal damage may already exist.
- Early diagnosis allows for treatments like laser therapy, injections, or surgery to be more effective.
- Timely treatment can slow or even prevent further vision loss.
- Delayed care increases the risk of blindness.
Risk factors for diabetic retinopathy
Anyone with diabetes can develop retinopathy, but certain factors increase the risk:
- Having diabetes for a long time (the longer you have it, the higher the risk).
- Poor blood sugar control.
- High blood pressure or high cholesterol.
- Pregnancy (diabetic retinopathy may worsen during pregnancy).
- Smoking.
How to protect your eyes?
Protecting your vision starts with proactive care. Here are some steps you can take:
- Get regular eye exams: A dilated eye exam once a year can detect retinopathy early, even before symptoms appear.
- Manage your blood sugar: Keeping blood sugar within target range slows the progression of eye damage.
- Control blood pressure and cholesterol: Both contribute to blood vessel health in the retina.
- Quit smoking: Smoking reduces blood circulation, making complications worse.
- Adopt a healthy lifestyle: Balanced diet, regular exercise, and proper medication compliance can make a huge difference.
When to see a doctor immediately?
Seek urgent medical attention if you notice:
- Sudden vision loss.
- A sudden increase in floaters or flashes of light.
- Severe or rapidly worsening blurred vision.
- Dark or empty areas appear suddenly in your vision.
These may indicate a retinal bleed or detachment, which requires immediate intervention.
Treatments available
If detected early, diabetic retinopathy can be managed effectively. Treatment options include:
- Laser Photocoagulation: Seals leaking blood vessels to prevent vision loss.
- Anti-VEGF Injections: Medications injected into the eye to reduce swelling and prevent abnormal vessel growth.
- Vitrectomy Surgery: Removes blood or scar tissue from the vitreous gel to restore clearer vision.
Conclusion
Diabetic retinopathy is one of the leading causes of vision loss worldwide, but it doesn’t have to take away your eyesight. The key lies in being aware of the early warning signs and committing to regular eye check-ups. Even minor changes in your vision should never be ignored, as timely detection and proper treatment can make all the difference. By managing your diabetes effectively and seeking expert care, you can protect your eyes and maintain a clear, healthy vision for years to come.
At Krisha Eye Hospital, our team of specialists is dedicated to providing advanced eye care and early intervention for diabetic retinopathy. Book your comprehensive eye check-up today and take the first step toward safeguarding your vision.
Author bio
Dr. Dhwani Maheshwari, an esteemed ophthalmologist with over 10 years of experience, leads Krisha Eye hospital in Ahmedabad with a commitment to advanced, patient-centered eye care. Specializing in cataract and refractive surgery, Dr. Maheshwari has performed more than a thousand successful surgeries. Her expertise lies in phacoemulsification, a technique recognized for its precision in cataract treatment.
Dr. Maheshwari’s educational journey includes an MBBS from Smt. NHL MMC, a DOMS from M & J Institute of Ophthalmology, and a DNB in Ophthalmology from Mahatme Eye Bank Eye Hospital, Nagpur. She also completed a fellowship in phacoemulsification at Porecha Blindness Trust Hospital, further enhancing her surgical skills. In addition to her work at Krisha Eye Hospital, Dr. Maheshwari serves as a consultant ophthalmologist at Northstar Diagnostic Centre.
Under her leadership, Krisha Eye Hospital aims to bring all super specialties under one roof, offering comprehensive eye care solutions for all vision needs.
FAQs
Yes, while good control lowers the risk, long-term diabetes can still cause subtle retinal damage. Regular eye check-ups remain essential.
There is no fixed age, but the risk increases after having diabetes for 5–10 years, especially in people over 40.
Once retinal damage occurs, it usually cannot be reversed. However, early detection and treatment can halt or slow down further progression.
Not always. It may affect both eyes, but one eye can be more severely affected than the other.
Yes, but it depends on the severity of retinopathy. Your ophthalmologist will evaluate whether surgery is safe and beneficial for you.
At least once a year, but people with existing retinopathy may need exams every 3–6 months depending on severity.
Often, no. Many patients have normal vision until the disease has progressed. That’s why preventive screening is crucial.
Yes, pregnancy can accelerate progression. Pregnant women with diabetes should have more frequent eye examinations.
